
Min Lang, MD, MSc
Department of Radiology, Massachusetts General Hospital
Harvard Medical School

John Conklin, MD, MS
Department of Radiology, Massachusetts General Hospital
Harvard Medical School

Claire White-Dzuro, MD
Vanderbilt School of Medicine
Neuroimaging plays a truly critical role in the initial evaluation of acute stroke. Although noncontrast head CT, followed by CT angiography (CTA), has historically been the standard imaging algorithm, it is well established in the literature and clinically that MRI is more sensitive for diagnosing acute ischemic stroke. Specific MRI sequences can provide vital information to help guide patient treatment decisions, especially for those with delayed presentation. For example, diffusion-weighted imaging (DWI) and fluid-attenuated inversion recovery (FLAIR) sequences often offer a better estimate for the onset of ischemia in patients with wake-up stroke.
As noted in our original AJR manuscript, “Triage of Patients With Acute Stroke for Endovascular Therapy: Point—Moving Toward MRI-Based Acute Stroke Triage With Ultrafast Protocols [1],” identification of DWI and FLAIR mismatch on MRI is suggestive of ischemic stroke with a duration of less than 4.5 hours, which is an important patient selection criterion for IV tissue-plasminogen activator (tPA). Additionally, MRI remains superior to CT perfusion imaging (CTP) for assessment of parenchymal integrity, tissue viability, and ischemic core—all of which can help determine thrombectomy and late-window thrombolysis candidacy.
Despite MRI’s superiority, CT remains the most commonly performed exam for code-stroke evaluation for two reasons. First, CT scanners continue to be much more accessible than MRI machines in emergency department (ED) and inpatient settings. Secondly, the imaging time for a head CT is on the order of seconds, whereas a brain MRI typically takes 10-15 minutes, depending upon which sequences are included in the protocol. The longer scan time for MRI results in the patient being more prone to motion, which could degrade the examination’s sensitivity.
Yes, we learned from the THRACE (Mechanical Thrombectomy After Intravenous Alteplase Versus Alteplase Alone After Stroke) Trial that there was a significant difference in acquisition time of a few minutes between patients who underwent CT versus MRI as their first imaging examination [2]. However, this slight delay in acquisition did not impact workflow or outcomes. And while CT remains the faster modality, when it is paired with additional imaging (e.g., CTA and CTP), overall imaging time ends up similar to MRI.
MRI’s intrinsic advantages over CT for evaluating acute infarction, as well as ongoing technological advances, have led to increases in MRI utilization within the ED: 38% from 1999 to 2008, though a more modest 18% from 2012 to 2019 [3-4]. (An increasing number of hospitals are moving toward 24/7 on-site MRI availability to obtain certification from The Joint Commission for Comprehensive Stroke Center, too.) In addition, newer ultrafast brain MRI protocols—comprised of T2/T2*-weighted, FLAIR, and DWI sequences—have been developed to further reduce acquisition times and increase the modality’s accessibility for acute stroke evaluation (Fig. 1).
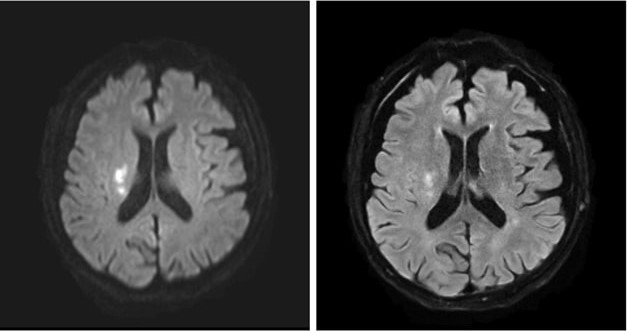
The total acquisition time of the ultrafast brain MRI protocol is approximately 2-3 minutes. This ultrafast protocol uses the multi-shot echoplanar imaging (EPI) technique, a highly efficient interleaved EPI technique using multiple excitations, to decrease geometric distortion and increase SNR. Recent clinical validation of the ultrafast brain MRI protocol published in the American Journal of Neuroradiology showed similar sensitivity for detecting acute intracranial findings and acute ischemic infarct as compared to standard brain MRI protocol [5]. Motion artifacts were also significantly reduced on the ultrafast protocol images. Application of deep learning-assisted reconstruction techniques will only continue to improve image quality and SNR, increasing the confidence of radiologists’ interpretations.
CT will remain the first imaging modality for any unstable patient, as well as for patients where MRI is contraindicated or where a facility faces limited scanner availability. But look at all the benefits of choosing MRI over CT for initial acute infarct screening, including:
- Differentiating stroke from mimickers
- Migraine
- Seizure
- Demyelinating process
- Infection
- Neoplastic process
- No radiation
- Lower risk for hypersensitivity reaction to gadolinium-based contrast agents
To conclude, with newer MR acceleration techniques, ultrafast MRI-based acute stroke evaluation has been shown to be fast, safe, and accurate. Therefore, MRI should be considered a suitable initial triage imaging modality for the appropriate patient and facility.
References
- Lang M, Conklin J. Triage of patients with acute stroke for endovascular therapy: point—moving toward MRI-based acute stroke triage with ultrafast protocols. AJR May 2024. doi: 10.2214/AJR.24.31303
- Provost C, Soudant M, Legrand L, et al. Magnetic resonance imaging or computed tomography before treatment in acute ischemic stroke. Stroke 2019; 50:659-664
- Burke JF, Kerber KA, Iwashyna TJ, Morgenstern LB. Wide variation and rising utilization of stroke magnetic resonance imaging: data from 11 states. Ann Neurol 2012; 71:179-85
- Wang JJ, Pelzl CE, Boltyenkov A, et al. Updated trends, disparities, and clinical impact of neuroimaging utilization in ischemic stroke in the Medicare population: 2012 to 2019. J Am Coll Radiol 2022; 19:854-865
- Lang M, Clifford B, Lo WC, et al. Clinical evaluation of a 2-minute ultrafast brain MR protocol for evaluation of acute pathology in the emergency and inpatient settings. Am J Neuroradiol Mar 2024. doi:10.3174/ajnr.A8143