
Athanasios Pavlou, MD
University of Maryland School of Medicine
R Adams Cowley Shock Trauma Center
Patient History
31-year-old female with no significant past medical history presented with multiple injuries after a motor vehicle accident. On arrival, the patient was conscious and moving her upper extremities but progressively developed lethargy.
Imaging Findings—Radiographs and CT Scan
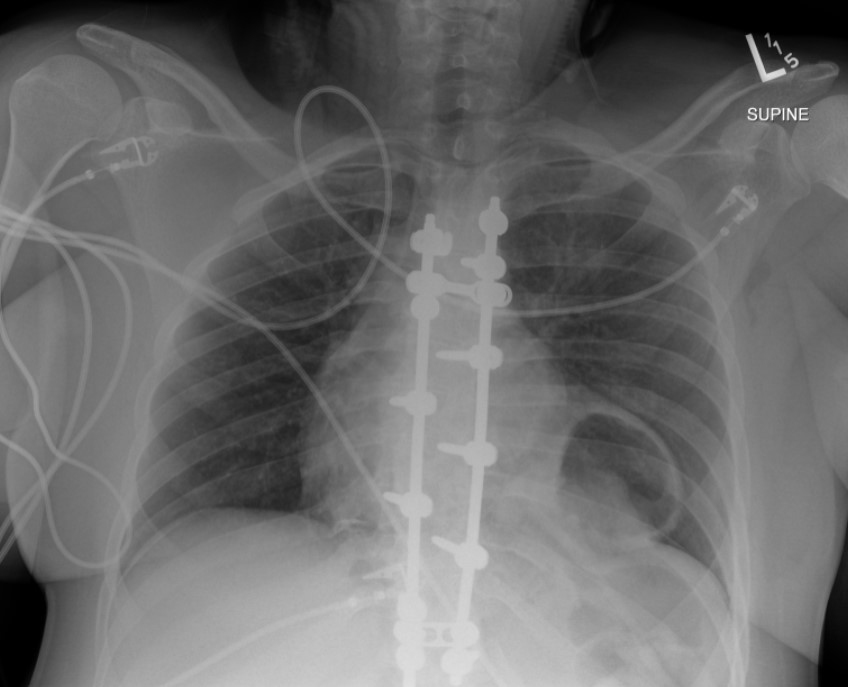
The initial chest radiograph (Figure 1) demonstrated a rounded retrocardiac partially lucent mass interpreted as a hiatal hernia.
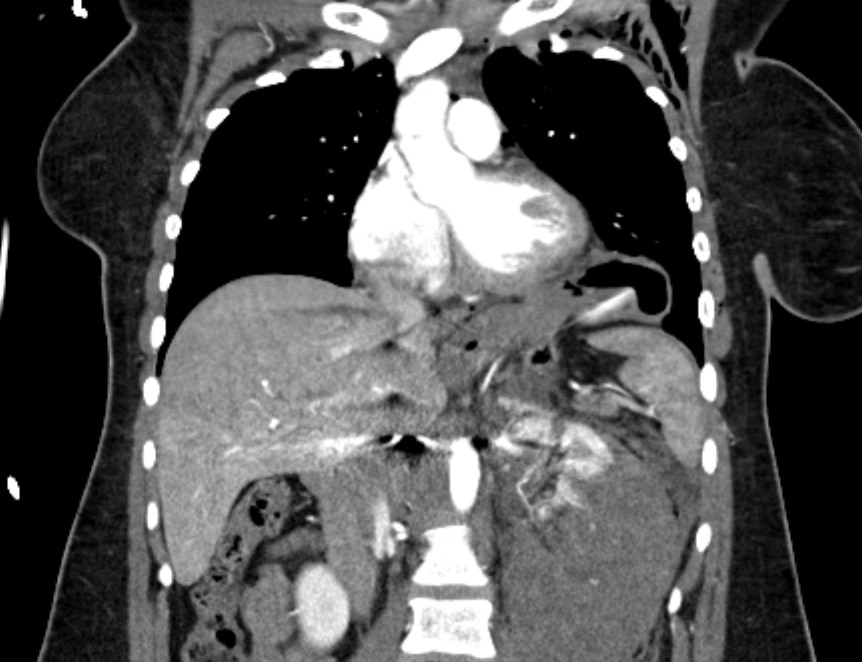
CT scan (Figure 2) revealed multiple clinically significant injuries, including a high-grade left renal injury. The stomach was elevated into the left hemithorax which was interpreted as the consequence of diaphragmatic eventration; medial diaphragm free edge was not appreciated.
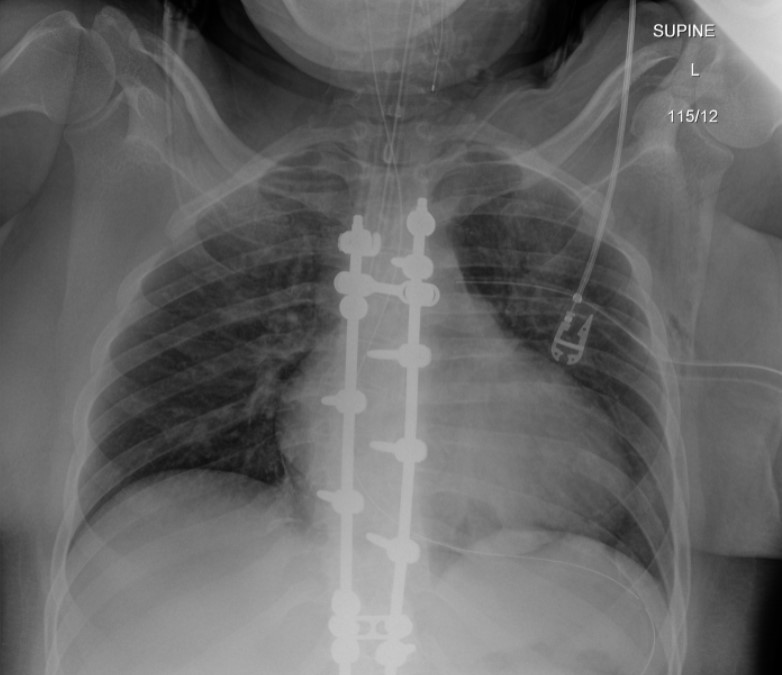
Postintubation radiograph (Figure 3) showed resolution of the retrocardiac mass with normal appearance of the diaphragm contour.
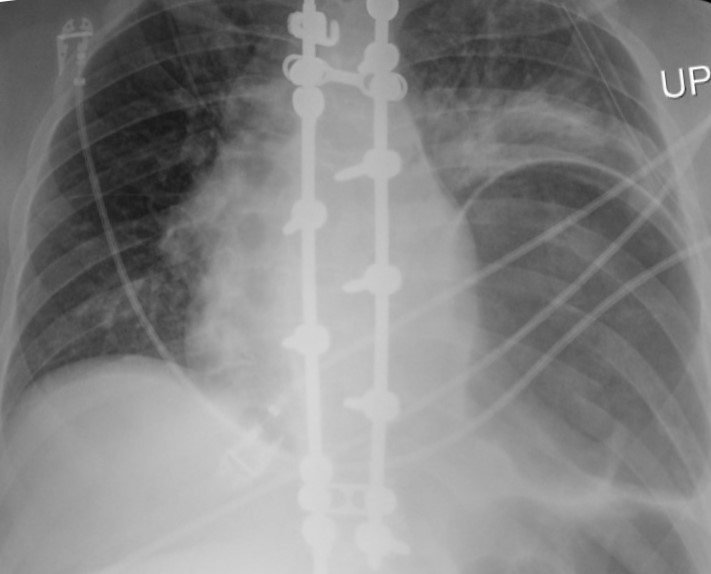
The patient subsequently underwent laparotomy for surgical repair of the renal injury. The follow-up radiograph (Figure 4) after extubation showed a recurrent lower left hemithorax partially lucent mass, increased in size compared to the initial radiograph.
Which Is the Correct Diagnosis? Click on the arrows to reveal the correct answer.
Phrenic Nerve Injury
Incorrect. Please try again.
Congenital diaphragmatic hernia
Incorrect. Please try again.
Traumatic diaphragmatic injury
Correct! Read Further Discussion for more details.
Intraoperative diaphragmatic injury
Incorrect. Please try again.
Further Discussion
Traumatic diaphragmatic ruptures are infrequent with a reported incidence of 0.8-8% in patients who suffer blunt diaphragmatic trauma. They more commonly involve the posterolateral aspect of the left hemidiaphragm. Reported symptoms include chest or abdominal pain, dyspnea, cough, and even a presentation of hemodynamic instability.
The main radiographic finding suggesting diaphragmatic injury is the elevation of the “diaphragmatic contour” either with or without visualization of a herniating hollow viscus. This may be difficult to differentiate from preexisting hiatal hernia, basilar atelectasis, diaphragmatic eventration, congenital hernias, and phrenic nerve injury which may have a similar appearance. Furthermore, as with our case, positive pressure ventilation may lead to delayed diagnosis due to temporary reduction of the intraabdominal contents. The reported rate of missed diaphragmatic injury on chest radiographs is variable and ranges from 12 to 66%. CT has higher sensitivity and specificity for the diagnosis of diaphragmatic injuries. CT findings include visualization of the discontinuity of the diaphragm (73% sensitivity, 90% specificity), intrathoracic herniation of viscera (55% sensitivity,100% specificity), the collar sign (63% sensitivity, 100% specificity), which refers to a waist like constriction of the herniated viscera where it extends through the diaphragmatic defect, and the dependent viscera sign (90% sensitivity, 100% specificity) which describes the positioning of the abdominal viscera directly anterior to the posterior ribs due to loss of the diaphragmatic structural support.
Management of blunt diaphragmatic injury is surgical repair. Laparotomy or thoracotomy with direct suturing or surgical mesh is the mainstay of treatment.
The prognosis is favorable if diagnosed early and repaired. Missed injuries can lead to delayed herniation of abdominal viscera with resulting morbidity and mortality due to the risk of strangulation.
Points InPractice
- Radiographic diagnosis of blunt left diaphragmatic injury may be suggested by elevation of the “diaphragmatic contour,” which can be misinterpreted as the result of other abnormalities.
- Positive pressure ventilation can reduce the herniated viscera into the abdominal cavity and conceal the radiographic findings of a diaphragmatic injury.
- In the setting of acute trauma, CT finding of intrathoracic herniation of abdominal contents has very high specificity for diaphragmatic injury and should be managed as such until proven otherwise.
References
- Hammer MM, Raptis DA, Mellnick VM, et al. Traumatic injuries of the diaphragm: overview of imaging findings and diagnosis. Abdom Radiol 2017; 42:1020–1027
- Iochum S, Ludig T, Walter F, et al. Imaging of diaphragmatic injury: a diagnostic challenge? RadioGraphics 2002; 22:S103–S116
- Sliker CW. Imaging of diaphragm injuries. Radiol Clin N America 2006; 44:199–211
- Zarour AM, El-Menyar A, Al-Thani H, et al. Presentations and outcomes in patients with traumatic diaphragmatic injury: a 15-year experience. Journ Trauma Acute Care Surg 2013; 74:1392–1398
- McDonald AA, Robinson BRH, Alarcon L, et al. Evaluation and management of traumatic diaphragmatic injuries: a practice management guideline from the Eastern Association for the Surgery of Trauma. Journ Trauma Acute Care Surg 2018; 85:198–207