The American Roentgen Ray Society (ARRS) proudly announces publication of the inaugural issue of its brand-new, peer-reviewed radiology journal: Roentgen Ray Review.
Marking the 125th anniversary of North America’s very first radiological society, ARRS’ Roentgen Ray Review (R3 for short) will continue to publish image-rich, clinically relevant content each week at R3journal.org.
Edited by John R. Leyendecker, MD, R3’s Pictorial Essays, Clinical Practice Challenges, Case-Based Reviews, Case Reports, and unique article formats like “Don’t Miss This” enable today’s working radiologists to integrate critical knowledge into imaging practices that continue to grow in both volume and complexity. Already, R3 is keeping busy ARRS members up to date on the latest developments in the specialty without compromising their demanding workflow routines.
Among the Volume 1, Issue 1 Roentgen Ray Review articles that our membership can access any time and anywhere are a few that exemplify ARRS’ mission:
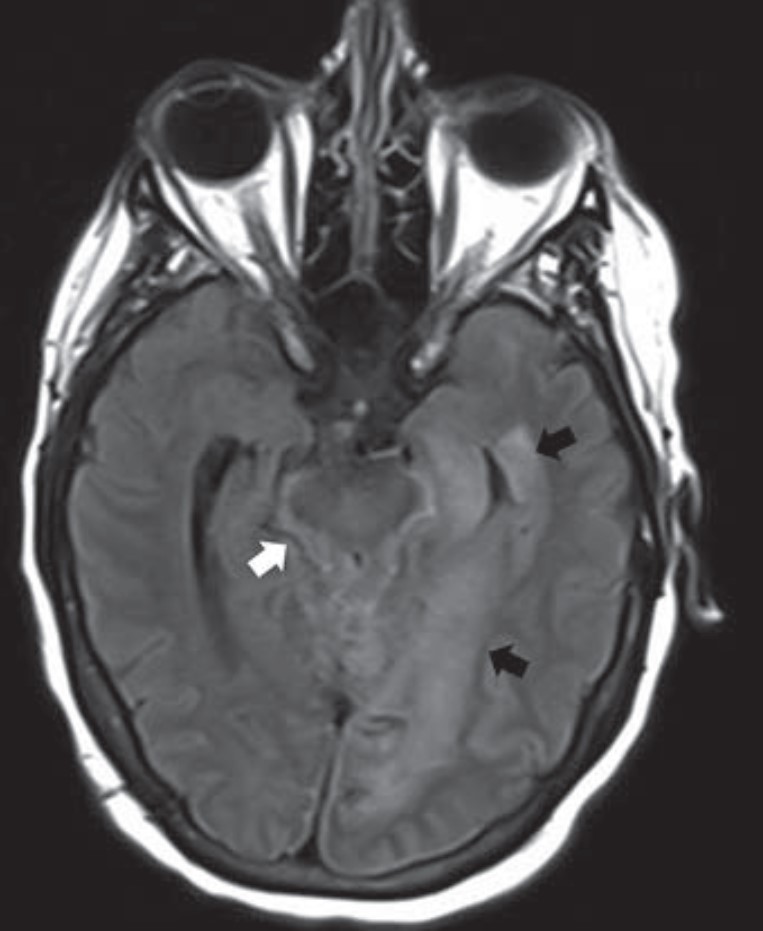
Overview of Imaging Intracranial Infections
The manifestations of CNS infections are myriad, including diffuse (meningitis, encephalitis, ventriculitis), focal (abscess, empyema), and other special presentations, especially in immunocompromised patients. Diagnosing CNS infections is decidedly multidisciplinary, and as “Overview of Imaging Intracranial Infections” points out, radiology’s contribution to the clinical workup of a patient is paramount. The Roentgen Ray Review’s first entry in its Categorical Course Highlight series, this CME credit article focused on key confounders details how CT and MRI with FLAIR sequencing and DWI can focus your differential diagnosis—ultimately streamlining additional testing and management decisions by the clinical team (Fig. 1).
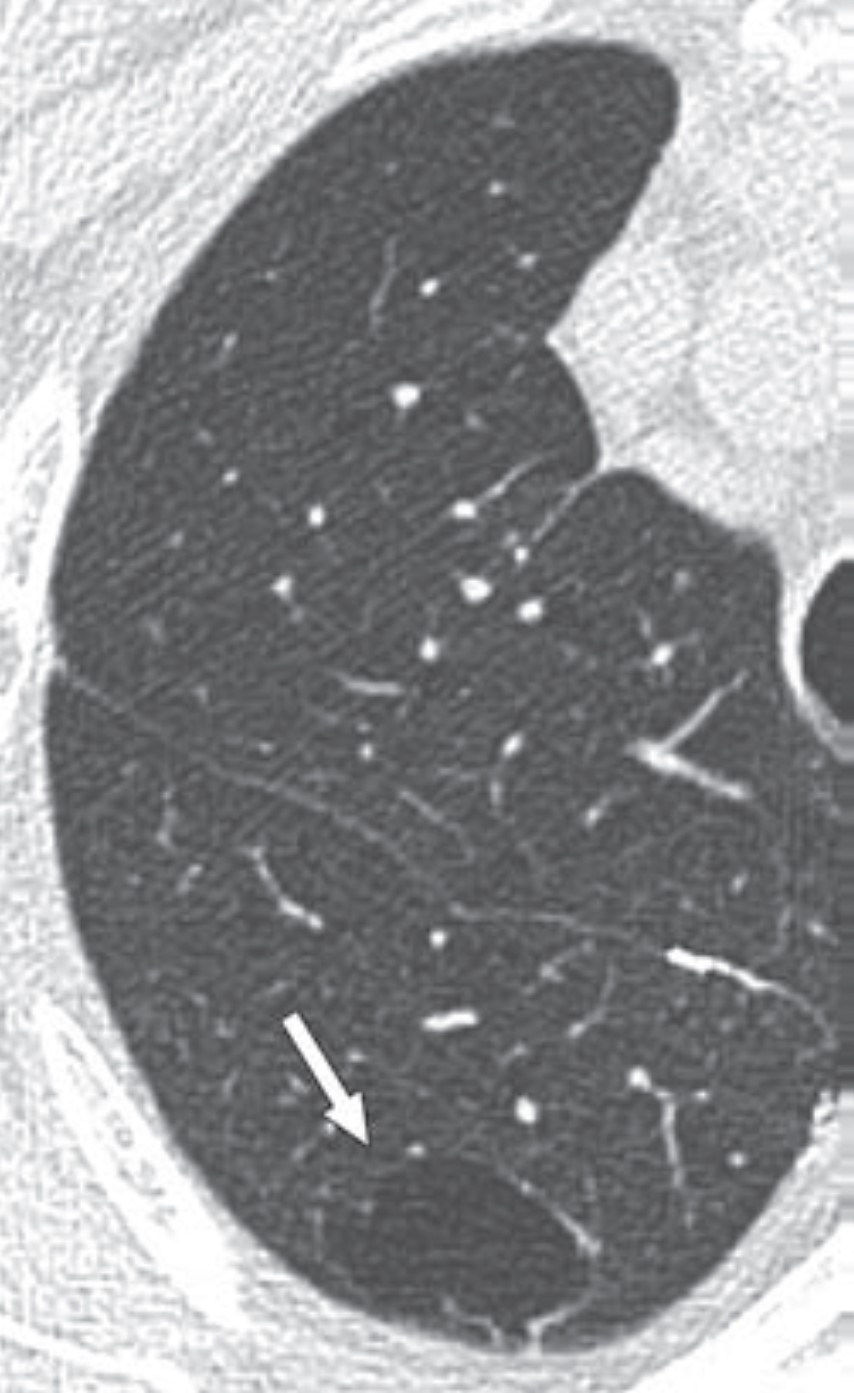
Approach to the Lung Cyst With Nodule
Because their imaging features can overlap with benign entities (bullae, fibrosis, bronchiectasis, etc.), lung cancers associated with cystic spaces are often diagnosed at later stages than cancers presenting as solid nodules. Compared to Lung-RADS version 1.1, Lung-RADS v2022’s updated classification and management criteria offer the potential for earlier detection and treatment of cystic cancers. This first Roentgen Ray Review Clinical Practice Challenge with CME tests readers on appropriate management of an atypical pulmonary cyst in a 66-year-old man with a 40-pack-year smoking history who had undergone right upper lobectomy for stage I lung cancer a decade earlier (Fig. 2).
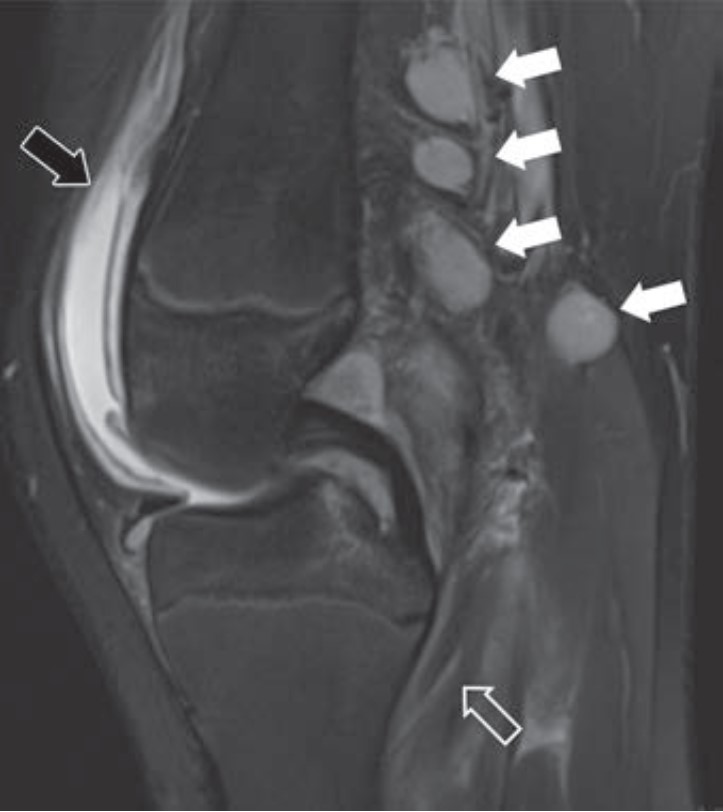
A Downward Spiral of Knee Pain and Swelling: Use of MRI to Distinguish Lyme Arthritis From Other Pediatric Arthritides
Clinical features of Lyme arthritis overlap with those of both septic arthritis and juvenile idiopathic arthritis, making the diagnosis of Lyme arthritis challenging. As “A Downward Spiral of Knee Pain and Swelling: Use of MRI to Distinguish Lyme Arthritis From Other Pediatric Arthritides” shows, MRI can help differentiate Lyme arthritis of the knee from other entities when certain imaging features, such as popliteal adenopathy, myositis, and lack of subcutaneous edema, are present. This first Roentgen Ray Review Case Report concerns a 13-year-old boy with a 1-month history of knee pain and swelling (Fig. 3).
Crucial but Often Unrecognized Radiologic Signs in Thoracic Imaging
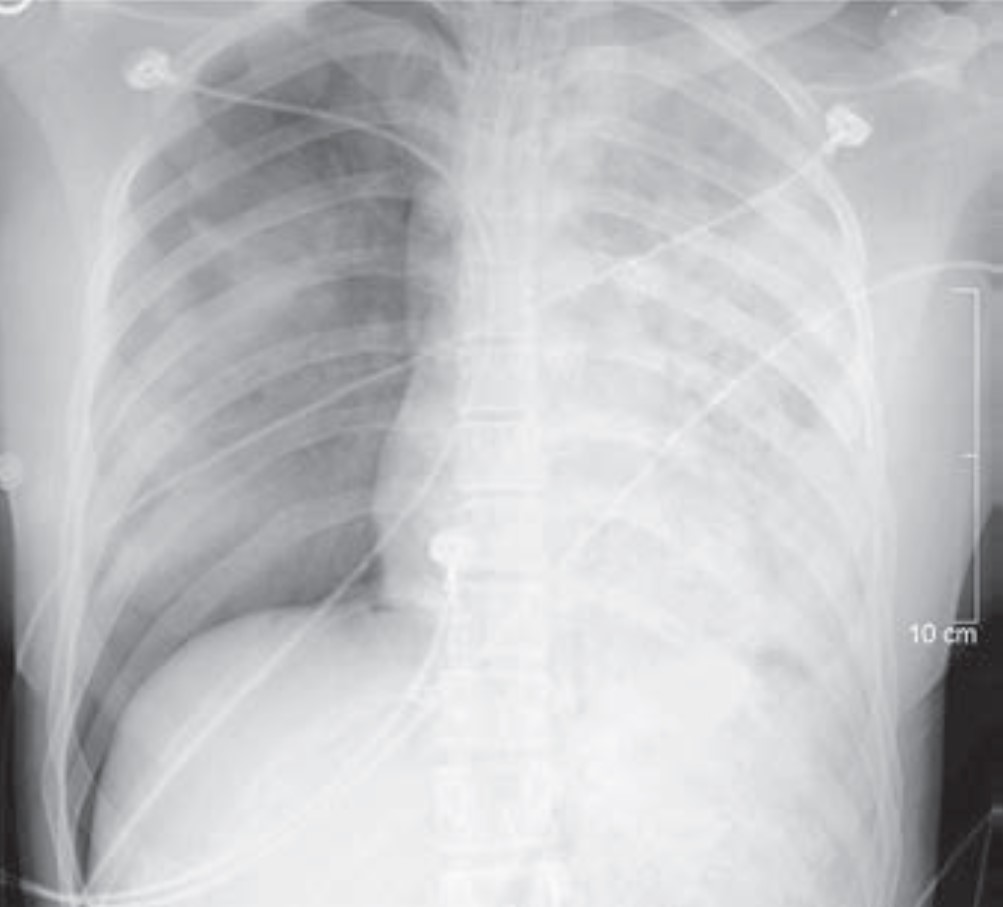
Despite its limitations, the chest radiograph is the world’s most frequently ordered and performed diagnostic imaging examination. However, accurately interpretating the chest radiograph remains challenging. “Crucial but Often Unrecognized Radiologic Signs in Thoracic Imaging” is the first of a two-part R3 Case-Based Review with credit highlighting key chest signs radiologists should recognize. Mark S. Parker, MD, presents six unknown cases of underlying abnormalities affecting the lungs, pleura, and mediastinum to help clinically steer your differential diagnosis (Fig. 4).
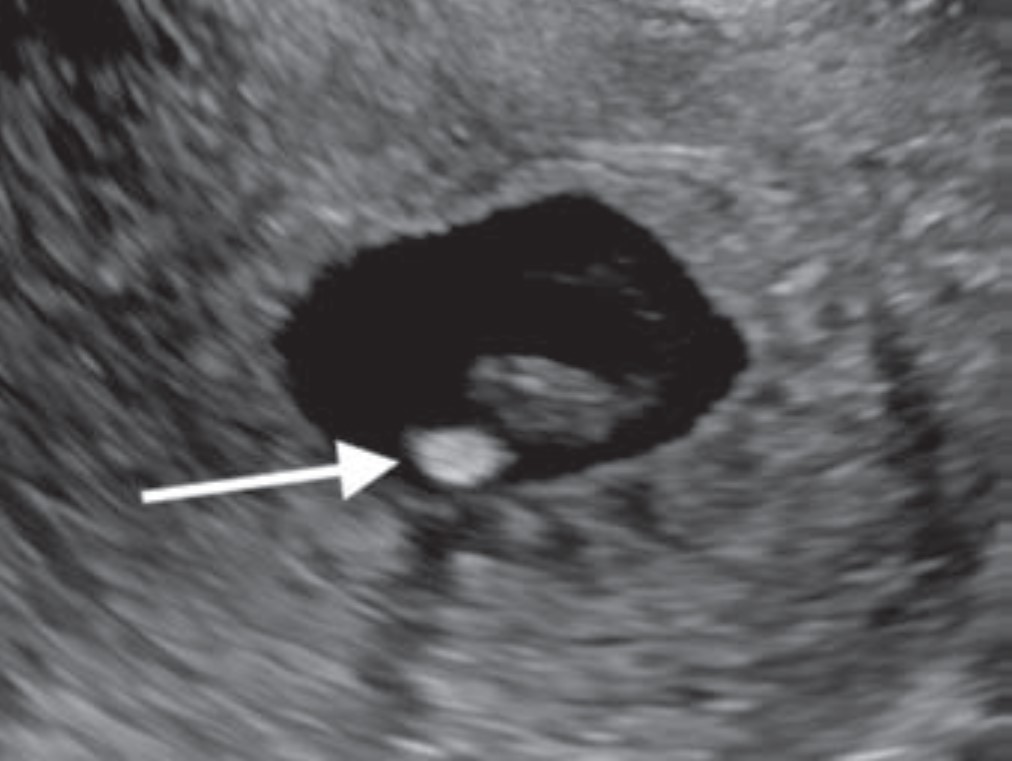
First-Trimester OB Imaging in the Emergency Setting
Radiologists play a key role in detecting early pregnancy, assessing cardiac activity and gestation location, as well as evaluating for complications in the acute setting. Knowledge of potential technical errors in image acquisition and an understanding of possible ectopic implantation locations are also necessary to optimize care of the pregnant patient in the first trimester. “First-Trimester OB Imaging in the Emergency Setting” reviews the pearls and pitfalls of first-trimester ultrasound—early pregnancy development, early pregnancy loss, intrauterine pregnancy of unknown location, ectopic pregnancy—applying the 2024 Society of Radiologists in Ultrasound Consensus Conference’s recommended lexicon throughout (Fig. 5).
Lateral Trochlear Osteochondritis Dissecans of the Elbow: A Rare and Subtle Finding With Important Implications for Management
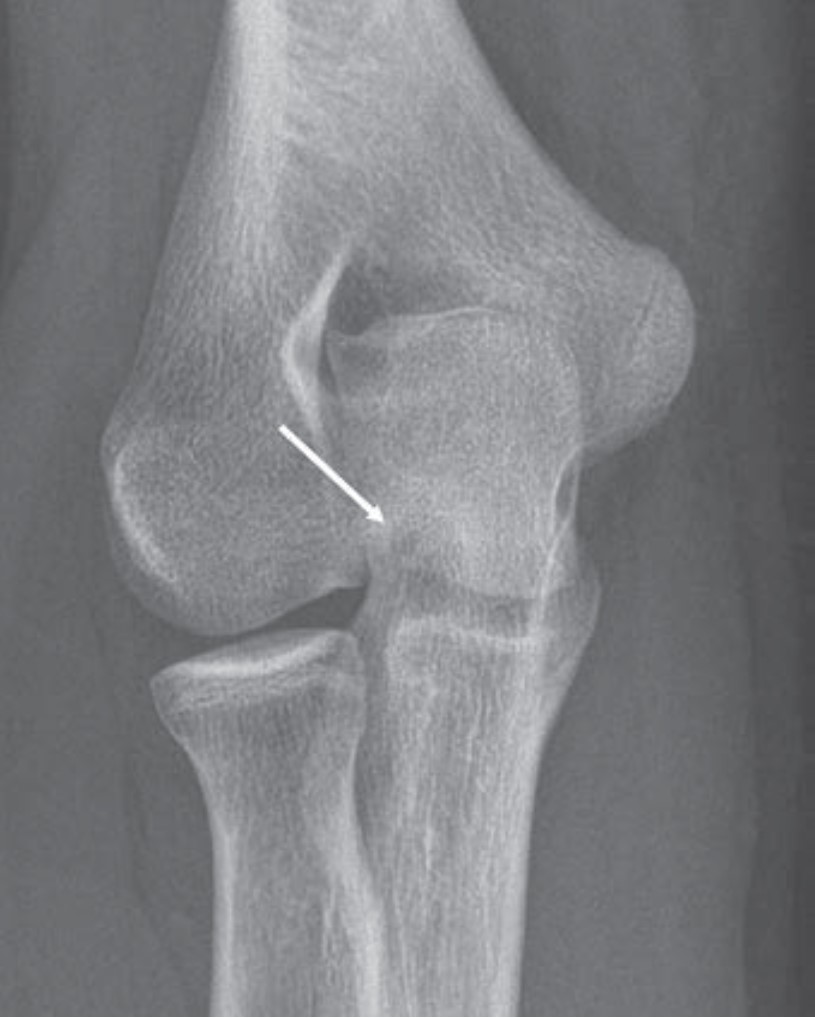
Given the overlapping ulnar anatomy and subtlety of its radiologic features, even experienced radiologists can miss lateral trochlear osteochondritis dissecans (OCD) of the elbow. As the first Don’t Miss This article in R3 notes, early identification of lateral trochlear OCD allows for appropriate activity modification, as well as timely intervention to mitigate lasting disability (Fig. 6).
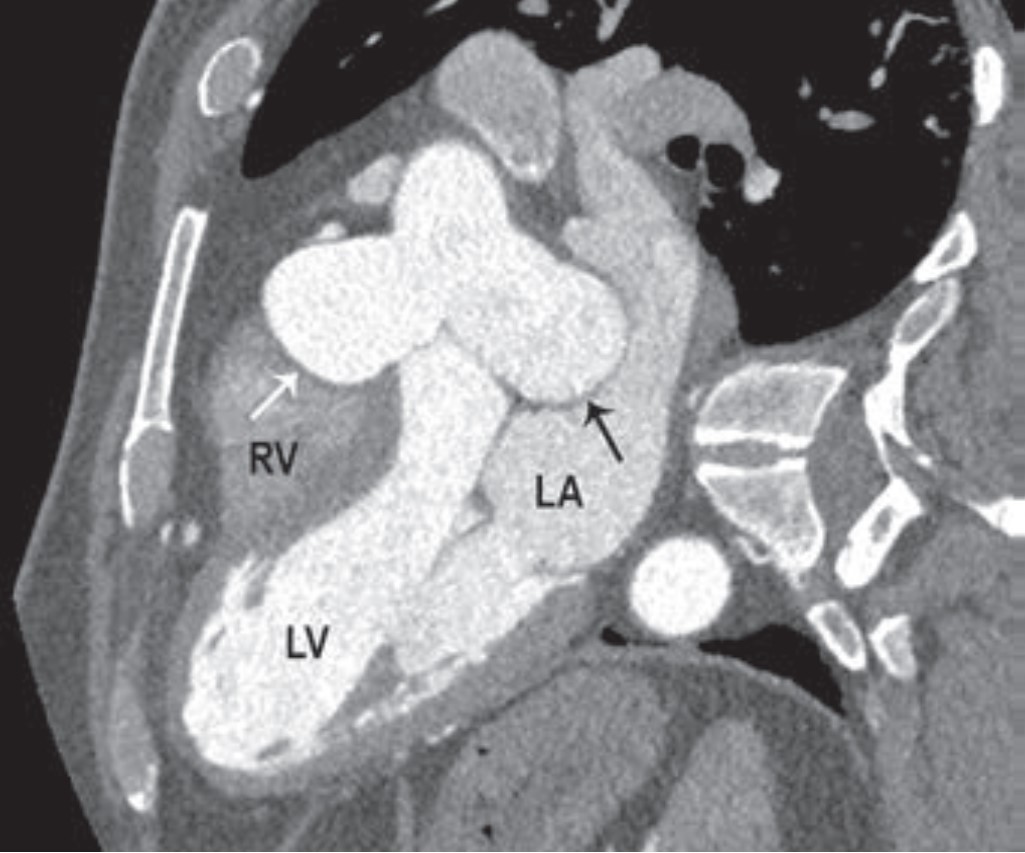
Coronary Artery Displacement and Narrowing on CT in the Setting of Giant Sinus of Valsalva Aneurysms
Whereas aortic valve regurgitation and rupture are known complications of sinus of Valsalva aneurysm, this Roentgen Ray Review Case Report illustrates that cardiac ischemia can be a manifestation, too. Presenting a 54-year-old man with large aneurysms involving all three aortic sinuses, “Coronary Artery Displacement and Narrowing on CT in the Setting of Giant Sinus of Valsalva Aneurysms” also illustrates the modality’s value in complex anatomical depictions for proper surgical planning (Fig. 7).