The American Roentgen Ray Society (ARRS) was but a teenager when the city of Boston, MA, first hosted an ARRS Annual Meeting. Dr. Henry Khunrath Pancoast (of “Pancoast lung tumor” fame) presided over that 1913 convocation in Boston, and North America’s first radiological society would return to the cradle of liberty for six more meetings before the 20th century was over.
The 2024 ARRS Annual Meeting at Boston’s John B. Hynes Veterans Memorial Convention Center delivered the same clinically relevant experience for which this society has long been heralded. From Sunday, May 5 to Thursday, May 9, radiologists of each practice type and every training level relished world-class instruction from trusted experts spanning every subspecialty.
Pioneers in asynchronous education a decade before COVID-19 changed everything, ARRS continues to offer both in-person and virtual registrants the most flexible meeting experience in radiology. From Instructional Courses and Scientific Sessions to Categorical Courses and Online Posters, all #ARRS24 attendees retain on-demand access to the complete program for an entire calendar year, learning and earning CME well into 2025.
And speaking of 2025, ARRS looks forward to delivering yet another singular experience at the Marriott Marquis Marina in San Diego, CA, next April 27–May 1.
After voting “yea” on a bylaw amendment to streamline the selection of committee chairs, the ARRS membership officially installed Angelisa Paladin, MD, of the University of Washington in Seattle as the 124th president of ARRS. Joining Dr. Paladin are the following newly elected ARRS officers for 2024–25: president-elect Deborah A. Baumgarten, MD, MPH; vice president Christine M. Glastonbury, MD; and secretary-treasurer Reginald F. Munden, MD, DMD, MBA.

Dr. Paladin succeeds Erik K. Paulson, MD, who presented this year’s coveted ARRS awards. The first laurels of the morning went to Philip Costello, MD, who was awarded the 2024 ARRS Gold Medal. The highest distinction bestowed by ARRS, our Gold Medal has been honoring distinguished service to radiology for more than four decades. Gaveled in as ARRS President during the 2018 Annual Meeting in Washington, DC, presently, Dr. Costello chairs the six vital scholarship programs of ARRS’ own Roentgen Fund®.

David M. Neager, MD, was then recognized as the 2024 ARRS Distinguished Educator. An engaging presence who motivates and impacts learners and colleagues alike, he exhibits his commitment to ARRS’ own educational initiatives—especially the Clinician Educators Development Program and Radiology Review Track—with attention to the needs and diversity of our members.

Next, ARRS was proud to recognize two recipients of 2024 ARRS Scholarships: Ian Mark, MD, of Mayo Clinic Minnesota and Evan Calabrese, MD, PhD, of Duke University Medical Center. Also provided by the Roentgen Fund, the ARRS Scholarship supports early-career faculty members pursuing radiological research that promises to change how medical imaging is practiced. A two-year grant totaling $180,000, the ARRS Scholarship aims to advance emerging scholars, as well as prepare them for positions of leadership.


Stephen Keevil, BIR President, Named Honorary Member
Professor Stephen F. Keevil, president of the British Institute of Radiology (BIR)—the oldest medical imaging society in the world—was recognized with honorary membership as part of ARRS’ Global Partner Society (GPS) program. Keevil served on the faculty for the 2024 ARRS Annual Meeting Global Exchange, “Screening Patient Pathways Across the Pond: Highlights and Challenges for Radiology in the UK and USA.” The GPS program was established to build long-standing relationships with key leaders and societies in the global imaging community to enhance understanding, raise awareness, and increase participation in programs and services. The Annual Meeting Global Exchange incorporates one partner society annually into the educational and social fabric of the meeting, with ARRS reciprocating at the partner society’s meeting that year.

2024 AJR Luncheon with Figley and Rogers Journalism Fellows
During the American Journal of Roentgenology (AJR) Luncheon on Monday afternoon, Francis Baffour, MD, of Mayo Clinic in Rochester, MN, was honored as the 2024 Melvin M. Figley Fellow in Radiology Journalism, while Hyun Soo Ko, MD, of the Peter MacCallum Cancer Centre and Epworth Medical Imaging in Melbourne, Australia was recognized as the 2024 Lee F. Rogers International Fellow in Radiology Journalism.


Named for two distinguished Editors Emeriti of AJR, the Melvin Figley and Lee Rogers Fellowships offer practicing radiologists an unparalleled opportunity to learn the tenets of medical publishing via “the yellow journal”—the world’s longest continuously published radiology journal. Through hands-on experience with ARRS staff and AJR personnel—as well as personal apprenticeship with AJR’s 13th Editor of Chief, Andrew B. Rosenkrantz—Drs. Baffour and Ko will receive expert instruction in scientific writing and communication, manuscript preparation and editing, peer review processes, journalism ethics, and digital production and publication.
With Distinction: Award-Winning Scientific Research
The 2024 ARRS Annual Meeting hosted hundreds of electronic exhibits and abstracts presenting leading-edge research. Below are three highlights from our 2024 Scientific Program.
Mammograms Reveal Hidden Clues to Heart Health

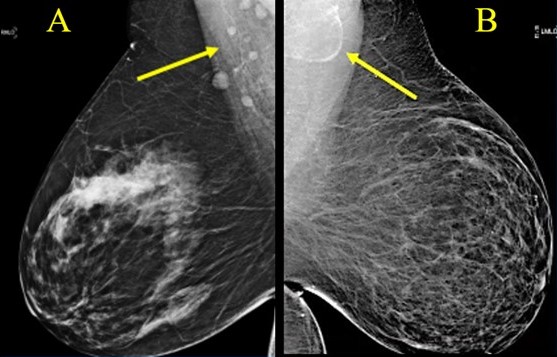
According to the Summa Cum Laude Award-Winning Online Poster presented during the 2024 ARRS Annual Meeting, fat-enlarged axillary nodes on screening mammograms can predict high cardiovascular disease (CVD) risk, Type 2 diabetes (T2DM), and hypertension (HTN).
“Incorporating fat-enlarged nodes into CVD risk models has the potential to improve CVD risk stratification without additional cost or additional testing,” said Jessica Rubino, MD, from Dartmouth Hitchcock Medical Center in Lebanon, NH. “Fat-enlarged axillary lymph nodes visualized on screening mammography may increase the ability to identify women who would benefit from CVD risk reduction strategies and more intensive risk assessment with coronary artery CT.”
Rubino et al. reviewed patients (women, 40–75 years) without known coronary artery disease who had a routine screening mammogram and cardiovascular risk factors available in the EMR within 1 year of the index mammogram (January 1, 2011–December 31, 2012). Evaluating major adverse cardiovascular events (MACE) within 10 years of the index mammogram, the researchers used clinical parameters at the time of the index mammogram to determine high estimated CVD risk via the pooled cohort equation (PCE) —defined by the American Heart Association as more than a 7.5% likelihood of MACE within 10 years. Two breast imagers evaluated screening mammograms to measure the length of the largest visible axillary LN in each breast in the mediolateral oblique view, analyzing the largest visible node for each patient. Logistic regression then examined associations between lymph node size, 10-year CVD risk, MACE, T2DM, HTN, low density lipoprotein (LDL), age, and BMI.
Ultimately, among 1,216 women included in this ARRS Annual Meeting Summa Cum Laude Scientific Poster, 907 (74.6%) had a visible axillary LN on the index mammogram, and 232 (19.1%) women had fat-enlarged nodes—defined as larger than 20 mm in length due to an expanded fatty hilum. Women with fat-enlarged nodes had a high risk of CVD defined by PCE (OR = 2.6, 95% CI 1.5–4.2), as well as a higher prevalence of T2DM (OR = 4, 95% CI 2.1–7.7) and HTN (OR = 2.5, 95% CI 1.6–4.0). Fat-enlarged nodes were also associated with a trend toward higher risk of MACE (OR = 1.7, 95% CI 0.9–3.1) and LDL (OR = 1.4, 95% CI 0.9–2.1).
“These results support further investigation of fat-enlarged lymph nodes,” Rubino added, “particularly with studies leveraging AI evaluation of mammographic fat-enlarged LNs and cardiometabolic disease.”
Detecting Accessory Infraglenoid Muscle in Teres Minor Fatty infiltration

The Magna Cum Laude Award-Winning Online Poster presented during the 2024 ARRS Annual Meeting showed a high prevalence (89%) of accessory infraglenoid muscle (AIGM) in patients with teres minor fatty infiltration (TMFI)—compared to those without (30%). Additionally, within the TMFI cohort, many AIGM abutted the axillary nerve with concomitant axillary neuropathy.
“These results stress the importance of looking for AIGM in the setting of TMFI, as TMFI on preoperative MRI has been associated with poor postsurgical outcomes,” said Jennifer Padwal, MD, from Stanford University Medical Center in California. “And the presence of AIGM on shoulder MRI could negate the need for additional imaging to evaluate the cause of TMFI.”
Padwal et al.’s institutional review of all shoulder MRIs yielded 100 patients with documented TMFI (76 men, 24 women; mean age, 58.6 years). For comparison, a respective sample of 100 shoulder MRIs in patients without TMFI (53 men, 47 women; mean age, 56.4 years) was obtained. All scans were consensus evaluated by two radiologists (one musculoskeletal attending with 25 years of experience, as well as a 4th-year radiology resident) for an AIGM with diagnostic confidence, noting muscle origin and insertion. In patients with TMFI, the distance between the AIGM and axillary nerve was measured, documenting any abnormal axillary nerve signal. TMFI was then graded via Goutallier classification, while the presence of atrophy and/or edema was noted.
Ultimately, in the ARRS Annual Meeting Magna Cum Laude Online Poster, TMFI was grade 1 in 33%, grade 2 in 32%, grade 3 in 13%, and grade 4 in 14%, with intramuscular edema in 33 and atrophy in 21 patients. AIGM was seen in 89/100 patients with TMFI; 30/100 patients without TMFI. In all cases, the AIGM originated from the inferior glenoid neck and inserted onto the humeral neck/proximal humeral diaphysis. The inferior margin of the AIGM in patients with TMFI touched the axillary nerve in 39 (46%), with abnormal signal in 23 (27%) patients.
Noncontrast Fluoroscopy Images Chronic Hypertension

The Cum Laude Award-Winning Online Poster presented during the 2024 ARRS Annual Meeting found that the noncontrast x-ray pulsatility index (XPI) method to evaluate and monitor pulmonary blood flow could improve clinical efficiency as a screening or diagnostic test, provide substantial financial benefits, and improve patient satisfaction.
“Additionally,” said Matthew Smith, MD, from Vanderbilt University Medical Center in Nashville, TN, “this easy-to-implement method can be performed by an x-ray technologist in an outpatient setting,”
Smith et al. enrolled volunteers suspected of chronic thromboembolic pulmonary hypertension (CTEPH) based on pulmonary scintigraphy and/or CTA. Fluoroscopic acquisition (70 kV, 30 frames/s) over an 8-second breath hold was performed in either RAO (30°) or LAO (40°) for the right and left lung, respectively. The temporal signal from each pixel was decomposed into individual frequency components via Fourier transform. The researchers then isolated heart rate signal oscillation using a band-pass filter and amplitude XPI mapped to form an image. Immediately following each fluoroscopic acquisition for spectral analysis, digital subtraction pulmonary angiography was performed with catheter-injected contrast in the same projection using standard protocols. Perfusion maps were segmented using a blinded manual technique, as well as a semi-automated threshold and region-growing method, while segmentation maps were compared using the Dice similarity coefficient—a statistical measurement of overlap.
Ultimately, in this ARRS Annual Meeting Cum Laude Scientific Poster, where noncontrast (XPI) and contrast pulmonary angiography images were obtained in 11 different lungs, all patients were able to perform satisfactory breath hold, despite moderate to severe disease. Direct comparison of segmentation maps revealed an average Dice score of 0.77, suggesting excellent agreement between XPI and pulmonary angiography maps in depicting regions of blood flow and, more importantly, lack of blood flow.